COVID: Reflections from the front line

Dr Aamir Saifuddin
Friday 13 March was the day it all became real. Before this, COVID-19 felt like a figment of imagination. Just something that was on the news and was affecting cruise ships and holidaymakers. People had become wary about shaking hands but it all seemed very precautionary. I’d recently completed six months working in the Liver Unit at King’s College Hospital in London and had started as a specialist registrar in the Gastroenterology Department two weeks previously, looking after complex hepatology and gastroenterology inpatients, conducting specialist clinics, and developing skills in gastroscopy and colonoscopy. Hospital services were continuing as normal and people were talking about COVID simply as a current affairs topic.
But on 13 March, I felt the atmosphere around the hospital change. In our department, the registrars, consultants and managers met to discuss how our working model might be affected by COVID. News alerts described rising European and British death tolls. The Prime Minister explained the need to ‘flatten the curve’ so our hospitals wouldn’t be overwhelmed. Medical conferences scheduled for June were being cancelled. The trust had begun to organise COVID Q+A and clinical simulation sessions. And rumours, though ultimately unfounded, began to circulate about doctors in London who were on life support machines. The stark reality of COVID, as a frontline medic, had hit.
In the subsequent days, as social distancing progressed to lockdown and daily mortality figures for King’s and the UK began to increase, the apprehension heightened. Before this, the most you might ‘catch’ from a patient (barring blood- borne viruses) was a vomiting bug. Now, you might feasibly catch a life- threatening virus that had seemingly already struck colleagues working only miles away. As the country was told to refrain from non-essential activities to reduce their risk, we were doing the exact opposite and travelling to virus hotspots every day, aware that King’s had the most cases in the country initially. We became aware that patients we had reviewed and examined without precautions, who had been previously admitted for other reasons, had tested positive, which brought a nervous wait for our own symptoms to potentially develop.
There was an acute sense that this was going to become an extraordinary few weeks. The roads suddenly emptied overnight. NHS workers were being offered free car parking, free taxi journeys, discounted takeaways and, even, razors to help stubble-free mask-fitting. The Nightingale Hospitals were being readied to treat an unfathomable potential surge of thousands of critically unwell patients (for comparison, large London hospitals normally have fewer than one hundred critical care beds). Non-urgent operations, procedures and clinics were cancelled; there would no longer even be the capacity to pursue socially distant video or phone consultations. Doctors, nurses, physios, and admin staff were all redeployed to bolster the manpower needed to manage the potential onslaught of sick patients. Many hadn’t worked on a medical ward for several years and were worried about how they’d cope with unwell COVID patients. The A+E Department was divided into ‘clean’ and ‘dirty’ sections. Feats of logistics and innovation increased intensive care capacity and wards became assigned as ‘COVID wards,’ including mine.
Simulation sessions were run for all staff, explaining how to use personal protective equipment (PPE) properly and how to deal with a COVID cardiac arrest. The alien concept of not performing immediate chest compressions if a patient had arrested needed to be drilled in – the risk of virus being expelled from the chest is too high unless everyone in the room is wearing full PPE. A nurse or doctor might find a patient suddenly not breathing and, harrowingly, have to leave to put on their own protective equipment before being able to help. During this already highly stressful scenario, specific care would also need to be taken when passing equipment in and out of the room to minimise the risk of contamination. There was a constant fear about what ‘the peak’ might look like. We all envisaged scenes like those from Spain and Italy on the news: patients with breathing tubes and ventilators in corridors and car parks, A+E and intensive care departments bursting at the seams, physically and mentally exhausted doctors and nurses wondering when they might get some proper rest, and doctors needing to choose which patients would be allocated the limited ventilators. Everyone kept wondering if we were in ‘the calm before the storm.’ It was genuinely scary to think that might be us in the weeks to come.
Luckily the storm has, so far, been avoided. The various curve-flattening interventions seem to have achieved their primary aim of maintaining the NHS’s intensive care and ward capacity. Whilst we’ve clearly been very busy and ITUs have been filled to the brim, the horrors of other countries haven’t been replicated; so, whilst the numbers of deaths are tragic, this seems to be because of the virulence of the infection itself rather than because individuals haven’t received the best possible medical care.
I was a registrar (the level below consultant) on a COVID ward and admitted COVID patients from A+E for over two months, and I had the chance to reflect during the midst of this. Medicine is unwaveringly fascinating. Unfortunately, this fascination brings with it illness and death, which is part of our daily medical lives. However, it also brings treatment, recovery, a privileged glimpse into people’s lives when at their most vulnerable, and unparalleled gratitude, which is why we love doing it and why it’s the best job in the world. This fascination also means we are constantly learning and reflecting and are able to improve outcomes for future patients.
My first reflection is how interesting it has been to treat patients with a brand new disease. Generally in medicine, experience counts for everything. The more experience you have, the more honed are your diagnostic skills and understanding of the nuances of treatment. But everyone is now learning from the same starting point, picking up information from the news, journals, their own day-to-day experiences and the experiences of others. A crucial part of this is deciphering when a patient with new fever, cough or breathlessness has COVID, or heart failure, or a clot in the lung, or another infection, for example, all of which have very different, and sometimes opposing, treatments. We began to appreciate that some patients, particularly the elderly, may have none of these ‘classic’ symptoms but may simply be more drowsy or ‘off their food,’ for which the differential diagnosis was already huge, but life-threatening COVID was now possible. Early on, around the NHS, there will have been misdiagnoses, with biases towards COVID at the expense of other conditions, at times with catastrophic consequences. Unfortunately in medicine, mistakes can be catastrophic, but subsequent learning aims to prevent recurrence. Some of the initial thoughts about how to treat very unwell patients with COVID have entirely changed based on experience – how much intravenous fluid to give, how to optimally use ventilators, understanding how patients develop clots. These patients also deteriorate rapidly, talking to you comfortably in the morning then needing a ventilator by lunchtime. It has been an intriguing process as everyone from the most junior doctors to senior consultants can update their colleagues about something new they’ve learnt the previous evening that can help patients the following day.
We have looked after a range of patients on our ward, including a female in their late-20s who was stable the day before and then quickly became unable to breathe properly whilst we were reviewing her on the morning ward round – I’d not been ‘scared’ by a patient for some years, but this was quite early on in the pandemic and I had no idea how quickly she might further deteriorate. Seeing her oxygen levels worsen in front of our eyes was terrifying. Luckily, we were able to treat her on the ward instead of transferring for a ventilator. We also cared for quite elderly people, some of whom improved, some of whom unfortunately did not. Many of these patients had also suffered recent COVID- related bereavements, often of male spouses. We did manage to discharge home a 95-year-old Afro-Caribbean woman with dementia, which seems a triumph in retrospect.
Another major effect of the situation is how we are working together in the hospital. Despite the apprehension whilst sitting in my COVID simulation session (one of dozens held for all staff), the feeling of togetherness amongst the various participants who would never otherwise cross paths, including medical physicians, orthopaedic surgeons, dermatologists, fracture clinic nurses, physiotherapists, palliative care nurses and so on, all of different grades, was inspiring and highly motivating. It reminded me of that scene in Apollo 13 when the Flight Director overhears two NASA Directors say: ‘This could be the worst disaster NASA has ever experienced.’ And he interjects with: ‘With all due respect, sir, I believe this is going to be our finest hour.’ This camaraderie has continued and my adult COVID ward has had dermatologists, paediatricians, HIV doctors, sexual health nurses, endoscopy nurses and others redeployed, all pulling together and sharing expertise within these randomly assigned teams to achieve the best for our patients.
No COVID frontline reflections would be complete without a mention of ‘PPE’, the range of personal protective equipment used by all staff to protect ourselves from the virus. Sometimes a distant interaction won’t require ‘full PPE,’ but sometimes you might be performing chest physiotherapy or an endoscopy or be in an area, such as A+E or intensive care, with a high patient density, where the risk of exposure is very high and the highest level of protection is needed.
Tragically, many healthcare workers have died from COVID, many presumably having caught the virus from a patient, so this is a very emotive topic. A comment on government policy is outside the scope of this piece, but suffice to say that having a constant supply of PPE will be crucial for many months to come. The difficulty initially was the changing guidance based on new evidence, especially when advice was ‘downgraded’. Some, understandably, have found it hard to decrease the amount of protection used when one’s own health is so palpably at stake. This will lead to staff wearing ‘inappropriate levels’ of PPE, which may affect stock. This, unfortunately, is the reality and somehow needs to be taken account of as workers are entitled to feel protected.
A side-effect of PPE I hadn’t considered is how difficult it is to communicate whilst wearing a mask. Overnight last weekend, I led a cardiac arrest situation on a ward and it was tricky trying to communicate effectively with dozens of faceless colleagues. Similarly, the subtle facial expressions you use when breaking bad news and that face-to-face connection where you can feed off these expressions is obliterated. Relatives are seldom allowed to visit any more; when they do, it’s because a patient is terminal, and explaining this whilst wearing a mask, particularly once the patient has died, seems very inadequate. Most conversations we would normally have in person, such as when a patient deteriorates, or when discussing resuscitation status, are now done by phone, which, again, makes it hard to gauge non-verbal cues to determine how to tactfully progress the conversation.
Finally, the pandemic will change how we practise medicine for months, maybe years to come. There have been rapid innovations that have been waiting to happen for a long time, such as telephone and video consultations, remote medical meetings and using apps so patients can regularly interact with their clinical teams, along with more efficient working patterns and community initiatives to reduce hospital attendances. A silver lining is that development of this infrastructure has accelerated which will give patients more flexibility to access medical care.
In such a short space of time, the whole world has changed. I feel privileged and fortunate to be a doctor during this, both so I can directly help those in need and so I can still go to work and see friends, teach and support junior colleagues, experience the well-known ‘banter’ within a hospital – which only increases at times of crisis! – and be part of this huge, incredible NHS family. It remains personally scary because we still only see the sickest patients, undiluted by the vast majority who have mild symptoms. We’re in recovery mode now, trying to reinstate important services like urgent care for suspected cancer cases, whilst balancing the ongoing demand of COVID patients. We also need to ensure people with acute non-COVID illnesses aren’t deterred from attending A+E as they normally would. I’ve seen many patients in extremis who would clearly normally have sought help earlier had they not been worried about catching the virus, and A+E attendances are significantly decreased compared to normal, despite hospitals being well-equipped to help. There’s still so much to learn, not least the implications of infection on future immunity or the effects of relaxing lockdown measures. But the focus now is on minimising the harm to patients with non- COVID illnesses whilst being wary of a dreaded ‘second wave.’
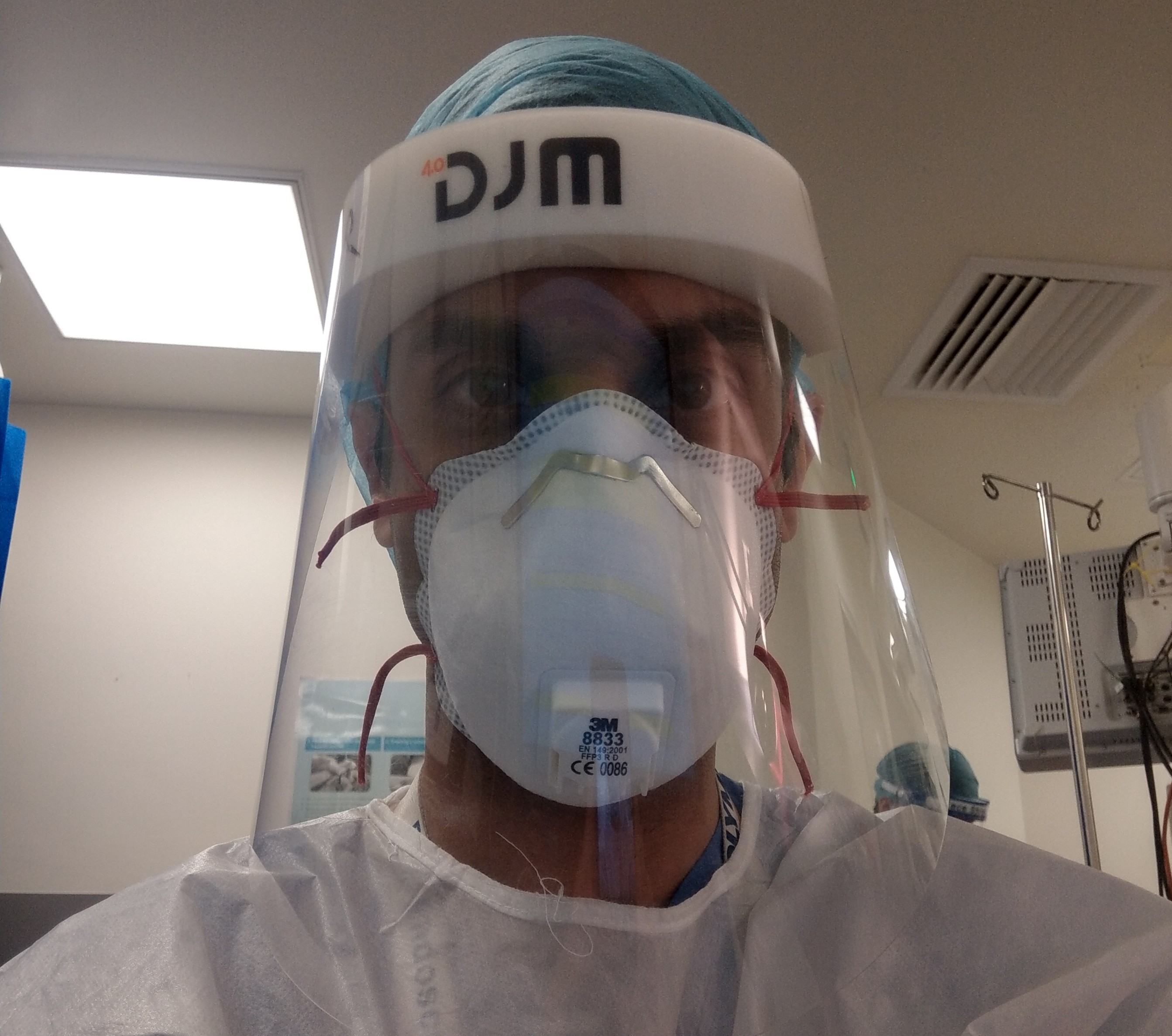
Dr Saifuddin took this photo of himself in PPE to show concerned family that he is wearing appropriate protective equipment at work
